
You eat protein. You lift weights. Your muscles are still slowly declining. The reason is 25 feet away from your biceps, and most health panels will never find it.
____________________________________________________________________________________________________________
You’re doing everything right.
You lift weights on average 3-4 days/week. You have elevated your protein consumption. You’ve studied the literature, taken the recommendations, and remained committed. You should theoretically be achieving better results based on your program.
However, there is an unsettling feeling.
Your strength hasn’t improved like it once did. Recovery is taking longer. There is a subtle fatigue that doesn’t match the amount of work you’re putting in. Quietly evident, yet noticeable. The majority of people believe that they just need to train harder, consume more protein, optimize their workouts, etc…
The typical response is that it is due to hormones or age. However, there is a much more accurate and actionable explanation for why you aren’t making progress and it begins in the gut. A gut microbiome test can help identify the root causes behind poor muscle response and recovery.
But what if the actual problem isn’t within your muscles?
What if the problem begins 25 feet from your muscles in your gut?
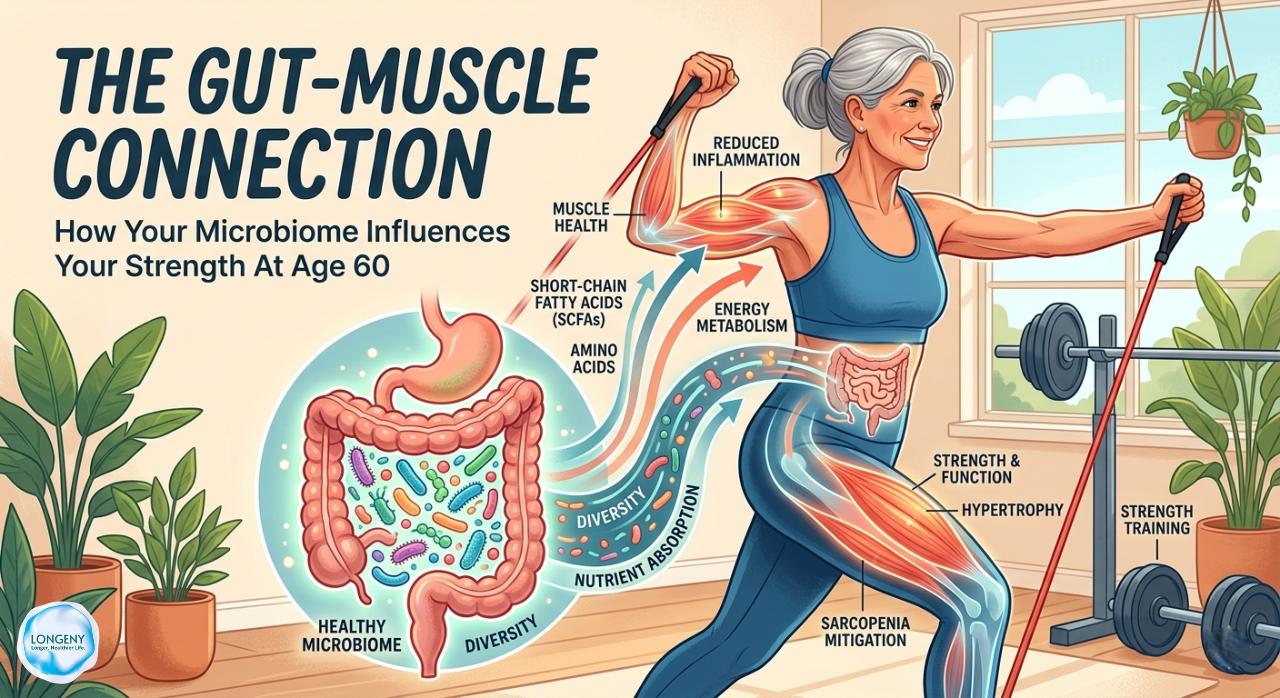
Muscle loss during aging is not only inevitable; it is also caused largely by what scientists call the gut-muscle axis (a bi-directional communication system between the gut microbiome and skeletal muscle) which most practitioners are using to inform how they think about aging. The implications are far greater than most people realize.
Understanding this axis may be the most important thing you can do to protect your strength, independence, and health span.
| 3–5% Muscle mass lost per decade from age 30 | 1–2% Muscle mass lost per year after 50, the rate doubles | ~50% Total muscle lost by the 9th decade |
Sarcopenia is the progressive and age-related loss of skeletal muscle mass, strength, and function. Sarcopenia occurs in approximately 5%-13% of adults aged 60. Sarcopenia affects approximately 45% of individuals aged 77-84. What is becoming increasingly apparent, however, is that muscle loss during aging is not solely due to aging. Muscle loss is primarily a result of biological processes that have begun to occur decades prior.
The stakes are significant: sarcopenia significantly increases the risk of falling, fracturing bones, hospitalization, cognitive decline, and premature death. Individuals with sarcopenia are at over double the risk of experiencing a fall than individuals without sarcopenia.
It is difficult to accept: muscle loss does not commence when you observe it. It commences when the physiological systems responsible for muscle, metabolic functions, inflammatory responses, and cellular energy production begin to deteriorate.
For many years, the narrative surrounding muscle health was simple.
Eat more protein. Train with weights. Remain active.
These suggestions are not incorrect. They are incomplete. They assume that the body will react predictably to these stimuli.
Increasingly, we are finding that the body does not always behave in this manner.
There are two individuals who follow the same nutritional plan, workout plan, and supplement regimen, and experience dramatically different results. One individual develops strength and recovers well. The second individual experiences fatigue, reaches a plateau early, and achieves very little strength gain.
The differences in these outcomes have been typically explained by genetics, commitment, or age. However, this type of explanation is no longer acceptable.
What we are actually viewing is a more complex process: the body’s ability to respond to nutrients and physical activity is mediated by numerous biological systems. One of the most important of these systems is the gut.
This is the point at which the concept of anabolic resistance comes in. As we age, the body is less capable of utilizing dietary protein to create new muscle proteins. Even though the dietary intake of protein is adequate or high, the muscles simply do not produce the expected levels of muscle protein synthesis.
The question is not whether protein is essential.
The question is: why is the body unable to utilize the protein adequately?
These numbers should concern you. Not because they are sensationalized but because they are consistently observed across high-quality research studies. If you are in your 40’s, this is the kind of data that should cause you to pause your screen and ask yourself: what changes are occurring in my body that I am currently unaware of?
| +72% Higher cardiovascular disease risk A study of 15,000 people found sarcopenia raises CVD incidence by 72% and cardiovascular event risk by 33% in middle-aged and older adults. | 4.5× Greater metabolic syndrome risk People with low muscle mass and high adiposity face 4.5× the risk of metabolic syndrome, 2.7× the risk of hypertension, and double the odds of type 2 diabetes. |
| 80% Of glucose uptake depends on muscle Skeletal muscle handles 80% of glucose disposal under normal insulin conditions. Less muscle = less capacity to clear blood sugar — regardless of diet. | 2.3× Higher fracture risk from a simple fall People with sarcopenia are 2.3× more likely to suffer a low-trauma fracture. |
Over the last few years, gut microbiome and muscle health research has gone from an unproven theory to an accepted scientific fact. The gut is no longer viewed as simply a passive digestive system. Instead, the gut microbiome is now recognized as an active metabolic organ that communicates with other organs, including skeletal muscle, through various mechanisms.
All microbiome disruptions are not created equal. Research continually shows that certain bacterial populations are important to muscle maintenance and loss, and therefore, a decrease in these populations serves as a biomarker of impending muscle loss.
Specifically, in patients suffering from sarcopenia, research has shown a consistent reduction in Faecalibacterium prausnitzii, Roseburia intestinalis, and Bifidobacterium longum, the primary producers of butyrate. Conversely, pro-inflammatory species from the Enterobacteriaceae family increase and produce LPS, which produces chronic low-grade inflammation and suppresses muscle repair.
The data from FMTs is compelling. In animal model studies, FMTs from young to old models resulted in grip strength gains of 30-50%. Initial human trials in sarcopenic elderly subjects showed that a single FMT resulted in significant reductions in key inflammatory markers and improvements in muscle mass and function for up to 24 weeks.
Equally as important is the bidirectional nature of the relationship. Exercise also changes the composition of the gut microbiome for the better. Studies have shown that exercise increases microbial diversity and increases the population of butyrate-producing species. The gut enhances the effectiveness of exercise, and exercise enhances the health of the gut.
However, if the gut microbiome is already severely disrupted, exercise alone may not be sufficient to disrupt the cycle of muscle loss.
Standard health panels usually test for markers such as cholesterol levels, glucose, and blood counts. Standard panels are very good for determining if there’s a disease problem; however, these tests tell you almost nothing about the gut-muscle axis, the factors that will drive your future strength trajectory, not your current disease status.
These tests don’t measure the diversity of microorganisms. They don’t measure the amount of short-chain fatty acids produced. They don’t measure gut permeability, nor do they measure the inflammatory signals that come out of your gut.
In other words, these tests won’t show you the upstream factors driving muscle loss.
When the first signs of the above become apparent in your standard marker tests, or, worse yet, in your ability to perform physically, the biological processes that caused those changes may have already been underway for years.
That’s why so many people feel like something is “wrong” long before their tests show it.
The biology is changing. The data just aren’t capturing it.
One of the key refrains in the field of longevity science is: decline is not an event. It is a trajectory. Muscle loss occurs slowly. It begins in the mid-30s.
|
|
The start of the decline is difficult to see. Muscle loss begins at 3-5% per decade from age thirty. Gut diversity is generally still high. However, through modern diet, chronic stress, and antibiotic use, this is beginning to erode. This is the best decade to create a baseline for your microbiome – before the decline becomes apparent. |
|
40s |
The accumulation phaseTraining recovery times begin to lengthen. Gut permeability is increasing. Low-grade inflammation becomes measurable. “Protein doesn’t work as well.” The anabolic resistance created by the decline of the microbiome is creating physiological issues. |
|
50s |
The critical windowRisk for sarcopenia increases. Gut diversity is typically lower than it was previously. SCFA production is significantly lower. The gut-muscle loop has been in motion for years. At this point, making targeted adjustments to it will produce measurable improvements in muscle mass and metabolic function. |
|
60s+ |
Still reversible with the right dataUp to 14% of adults in their early sixties experience sarcopenia. Sarcopenia rapidly increases with each additional decade. However, healthy older adults tend to have more diverse gut microbiomes than unhealthy older adults. Targeted microbiome intervention has been shown to improve muscle mass outcomes for older adults. |
What is often referred to as “age” is, in reality, in many instances, the culmination of previous declines.
Fortunately, this trajectory does not need to be set in stone.
Intervention programs focused on the microbiome have been demonstrated to improve muscle mass, reduce inflammation, and improve physical function in both younger and older adults.
This flips the conversation from inevitability to opportunity.
Since the gut is upstream, any interventions must be reflective of that.
You cannot possibly know what you should do without knowing what your microbiome looks like. A gut microbiome test India can help you understand how much diversity is in your microbiome, what its composition looks like, and how it is functioning. Any intervention you attempt, based solely upon symptoms, will be guesswork. How much diversity is in your microbiome? What is the composition of your microbiome? How is your microbiome functioning? Any intervention you attempt, based solely upon symptoms, will be guesswork. There could be two individuals who appear to be identical in terms of symptoms. Each individual would likely have an entirely different profile of microbes in their gut, therefore requiring completely different approaches.
At this point, the goal is to rebuild the ecosystem.
Your diet plays a crucial role. High fiber diets, especially those containing fiber from multiple plant sources, provide the nutrients necessary for beneficial bacteria to produce short-chain fatty acids. Fermented foods contain strains of microorganisms that help create balance. Foods rich in polyphenols serve as prebiotics, providing beneficial nutrients to specific strains of beneficial microorganisms.
Interestingly enough, regular exercise has a positive influence on the microbiome. Studies have shown that regular exercise increases the diversity of microorganisms and improves the production of metabolites that positively affect muscle function. There is a positive feedback loop here. Improved gut health will positively affect exercise results. Exercise, in turn, positively affects gut health.
There is certainly value in supplementation. However, that value can only be realized if it is based upon data. Probiotic supplements are one example. The benefits of probiotic supplements vary greatly depending on the strain. If you do not understand what is missing, supplementation is either ineffective or redundant.
For many years, age-related loss of muscle mass has been viewed as an unavoidable result of aging. However, with increasing amounts of evidence showing us that muscle loss isn’t simply a matter of how old you are, the framing of this issue is becoming increasingly hard to support.
In other words, what we now know is that while some biological factors are related to time, many of them can be directly related to the gut.
In no way does this mean that physical activity and diet aren’t critical to overall fitness. Rather, their effectiveness will depend on something that is foundational to all of our physical activity.
So rather than asking how much are you working out at the gym, the better, and therefore more effective question to be asking yourself is: Have you ever examined the foundation upon which your muscles were created?
People generally do nothing about the loss of strength in their muscles until they notice it.
By that point in time, the underlying processes that caused the decline in muscle strength have already been operating for 10 or more years.
If you look back at when the first signs of decline began to show up (and before those declines became visible), that is likely when the best opportunity existed to positively affect the process of losing strength. Using a more detailed, data-based approach to identify these early indicators will help give you the greatest opportunity to positively affect the potential for loss of strength.
LONGENY’s Gut and Metabolic Testing Panel was developed to provide this type of information.
The testing panel measures microbial composition and metabolic function, as well as inflammatory markers, providing a comprehensive view of the body’s health through analysis of a large number of biomarkers.
Furthermore, this testing panel doesn’t measure the biomarkers as separate individual data points; instead, the test measures them as part of a larger interconnected system.
Ultimately, strength at 60 is not just something that develops at 60. Rather, the development of strength at 60 is based on the quiet, consistent work of the biology that you’ve had for years.
And the gut may be one of the areas where you need to begin looking.

Anil K.C. is the founder of LONGENY, a precision health platform focused on extending healthspan, and longevity, through science-backed diagnostics, nutrition, and personalized care. A serial entrepreneur and host of the Brighter100 podcast, he translates complex longevity science into clear, actionable insights.

Anil K.C. is the founder of LONGENY, a precision health platform focused on extending healthspan, and longevity, through science-backed diagnostics, nutrition, and personalized care. A serial entrepreneur and host of the Brighter100 podcast, he translates complex longevity science into clear, actionable insights.
