
Your lab work is in. Your thyroid panel was a little low. Your hormone levels were “normal”. Yet you’re still tired all the time. Your cycle is irregular. Bloating occurs at the same time each month. Weight loss just doesn’t happen. Mood swings occur out of nowhere.
|
38 trillion microorganisms live in the human gut – roughly equal to the number of human cells in the body. Their collective genetic information is 150 times greater than the human genome. Sender et al., PLOS Biology, 2016 |
It’s not just you. It’s also possible that your physician hasn’t had the opportunity to have an honest conversation with you yet as to what could be causing your actual symptoms.
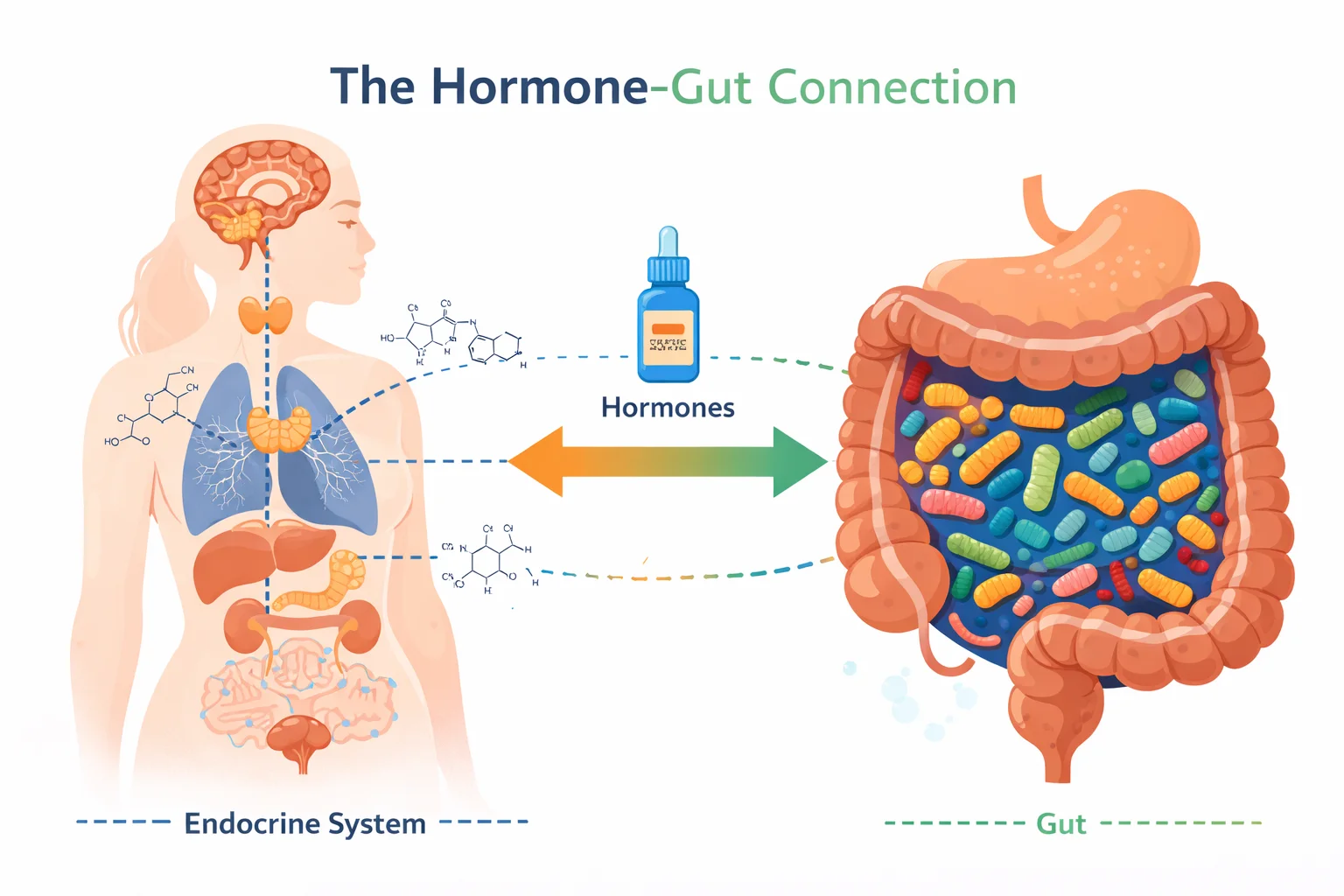
Most routine doctor visits miss something very important: your gut microbiome is a key regulator of your hormonal health. It’s not just a supporting role. It is a central player. Over the last ten years or so, the scientific research on this topic has been building rapidly, and it is becoming increasingly difficult to ignore.
In addition to being the site of digestion for nutrients from your food, there is an enormous amount of biochemical and biological activity occurring within the micro-ecosystem residing deep within your digestive tract. They do far more work than just digesting your lunch. In fact, many scientists have recently referred to this area as a “second organ” or more specifically, a “second endocrine system.”
Men and women with higher microbial diversity harbour significantly better sex hormone balance, testosterone in men, oestradiol in women.
Pakpahan et al., PeerJ, 2025; Gut Microbiota for Health, 2025
PCOS – Polycystic ovary syndrome, as a disorder of hormones, impacts an estimated 1 out of 5 women in India who are of childbearing age. Therefore, it has the potential to be one of the most common endocrine disorders within this population.
However, what is generally not discussed by clinicians is that there is significant evidence to suggest that women who experience PCOS consistently exhibit differences in their gut microbiomes when compared to healthy females; specifically, they often have lower diversity of bacteria present in their gut, imbalances in the ratio of bacteria found in the gut, and higher amounts of inflammatory species. Improving your gut health is a critical step in managing these systemic imbalances.”
A 2025 systematic review published in Frontiers in Microbiology demonstrated that the dysbiosis associated with metabolic syndrome overlapped significantly with that experienced by women with PCOS.
Insulin Resistance – Insulin resistance occurs in up to 70 percent of women with PCOS. The relationship between the gut and insulin resistance is direct. Dysbiosis can reduce the amount of short-chain fatty acids produced in the gut, such as butyrate. Butyrate is necessary for normal insulin sensitivity. Less butyrate means less insulin sensitivity. Less insulin sensitivity means increased androgen production. Increased androgen production causes greater severity of PCOS symptoms. This creates a cycle of continued deterioration.
“If you have PCOS and you’ve been told it’s just ‘hormonal’ or ‘genetic’ – this matters. The gut is a modifiable system. There are real levers you can pull.”
Leaky Gut – When the integrity of the lining of the small intestine is damaged, pieces of the cell walls of bacteria, specifically lipopolysaccharides (LPS) – enter the bloodstream. Once LPS enters the bloodstream, it triggers chronic low-grade systemic inflammation that travels throughout the entire body, including each endocrine gland (ovaries, thyroid, pancreas, adrenals).
Leaky gut does not scream its presence. Rather, it operates silently, causing damage over time (months, years) until symptoms are severe enough to warrant investigation.
Thyroid disorders in India
There are approximately forty-two million individuals in India who live with some form of thyroid disorder; this makes India have one of the largest numbers of individuals in the world affected by an endocrine condition. As well as being one of the most frequent forms of an endocrine condition, thyroid disorders also tend to be one of the most commonly misdiagnosed or undiagnosed until they reach late stages.
The connection between the gut-thyroid system
More so than many realize, the relationship between the gut and the thyroid system extends far beyond simply a physical connection. It has been demonstrated through research that the gut microbiome plays a critical role in regulating iodine absorption, selenium availability, and recycling of thyroid hormones (via enterohepatic circulation) all of which are important to ensure proper hormone production and conversion from the thyroid.
A 2024 study published in Nature Reviews Endocrinology found that autoimmune thyroid diseases – Hashimoto’s thyroiditis and Graves’ disease- were strongly related to gut dysbiosis, and that alterations to microbial populations could both occur before, during, and contribute to accelerating the onset of these diseases.
|
Autoimmune thyroid diseases affect 2–5% of the global population. A Mendelian randomisation study (2024) found a causal link between specific gut microbiota changes and autoimmune thyroiditis. Nature Reviews Endocrinology, 2024; Xiong et al., Front. Genetics, 2024 |
Plainly stated: Your gut produces and recycles nutrients your thyroid cannot function without. A disrupted microbiome is essentially starving your thyroid, regardless of whether your diet appears adequate or if standard blood tests indicate normal values.
Your gut and stress hormones have an ongoing dialogue. Under constant stress, the hypothalamic-pituitary-adrenal (HPA) axis will release corticosteroids (cortisol). Cortisol tells your gut to reduce good bacteria, increase gut permeability, and create conditions favoring dysbiosis. This intricate dialogue is part of the gut-brain axis, a bidirectional communication system that links the emotional and cognitive centers of the brain with peripheral intestinal functions.
“About 90 percent of the body’s serotonin is made in the gut. Mood problems, loss of stress-resistance, and sleep issues usually occur long before you see anything else go wrong with your gut.”
This isn’t just a footnote. Research has shown that gut microbes regulate the natural fluctuation of cortisol secretion throughout the day. When that balance is disrupted, so is cortisol fluctuation. Therefore, there is a biological basis for why you wake up at 3 am, crash mid-day, and feel like you’re always on but never get rested.
There is inflammation that ties all of these together. When LPS gets into systemic circulation through the leaky gut, it causes the production of pro-inflammatory cytokines (IL-6, TNF-α), some of which can pass through the blood-brain barrier, damaging insulin receptors, inhibiting thyroid hormone conversions, and interfering with ovarian functions at the same time. Inflammation does not single out one target. Rather, it targets many hormonal systems, causing all symptoms to amplify and making every attempt at treatment harder to continue.
Gastrointestinal and endocrine systems do not typically communicate with each other in a way that allows us to easily recognize how they are connected. Most commonly, we receive our clues as random events occurring at different times and in different aspects of our health that seem unrelated to each other.
Look for these patterns, either alone or in combination:
Bloating that worsens cyclically (typically around the premenstrual cycle or after prolonged exposure to high levels of stress.
|
1 in 3 people in India report weekly digestive discomfort. Over 135 million live with metabolic disease. Most have never had a gut microbiome test to identify the root cause of these symptoms.” |
Standard hormone panels are only capable of detecting established disease. Therefore, they are meant to identify when the thyroid has completely failed, when a person’s testosterone levels have dropped significantly, and when their estradiol levels are in the clinical range. In other words, they are unable to detect the functional imbalances of the gut that have silently contributed to hormonal disruptions for the previous 18 months.
In all cases, by the time a laboratory test identifies an abnormality in your hormones (or otherwise), the root cause of the dysfunction (the disordered gut microbe populations, the chronic inflammation, etc.) has existed for many years. These laboratory tests measure the consequences of the dysfunction, but do not address the underlying causes.
You may be experiencing severe disturbances in your gut microbiota (i.e., decreased species diversity; increased inflammatory cytokines; disrupted metabolic processes); yet all standard hormone panels would be normal. There is absolutely nothing wrong with conventional medicine. The issue here is merely that there exists a significant gap between what standard diagnostic testing was intended to identify and the actual physiological issues occurring in your body prior to the onset of clinically diagnosed disease.
Fortunately, there is substantial research supporting the fact that the human gut microbiota system is highly reactive. Dietary changes alone can lead to rapid shifts in the gut microbiota.
As follows is a summary of what the literature consistently supports:
Diversify Your Diet: Expand your consumption of diverse plants, not simply your supplement intake. Plant food diversity is the single greatest determinant of gut microbiota diversity. Consuming 30 or more different types of plant foods per week (including fruits and vegetables, legumes, whole grain products, nuts, seeds, and herbs) continually increases microbial diversity.
Indian diets, which include high amounts of legumes, fermented foods, and spices, provide many opportunities to increase microbial diversity. Utilize these resources.
Preserve traditional fermented foods: Fermented foods such as curd, kanji, idli batters, kimchi, and lacto-fermented pickles serve as excellent sources of prebiotics and probiotics. The estrobolome, in addition to feeding beneficial microbes, also provides a substrate for the production of short-chain fatty acids. Please do not substitute these nutrient-dense foods with processed foods.
Gradually reduce your consumption of ultra-processed foods, rather than attempting complete elimination. There is extensive evidence documenting the impact of consuming ultra-processed foods on disrupting microbial diversity. Rapidly reducing the amount of ultra-processed foods in your diet is far more important than achieving perfect avoidance over an extended period of time.
Disrupt the stress loop – at least in part, at the level of the gut. Since the stress-gut axis is bidirectional, stress reduction interventions directly influence the microbiome. For example, engaging in daily walking routines, limiting exposure to screens before bedtime, eating meals while disconnected from electronic devices, and engaging in relaxation techniques such as yoga and meditation have measurable influences on both gut composition and cortisol rhythm patterns.
Test first; don’t guess later. Unless you know your personal microbiome profile — including microbial diversity, inflammation biomarkers, estrobolome function, and insulin-related biochemical pathways attempts to alter your diet and lifestyle through trial-and-error methods are costly and ineffective. Precision requires knowledge of a baseline.
You can Read More Articles Here :
1. Gut-Muscle Connection That Nobody’s Talking About: How Your Microbiome Influences Your Strength At Age-60.
2. Acid Reflux and GERD: Why Does It Happen? Not Just Too Much Acid, Plus How to Get Evidence-Based Relief.
3.Why You’re Bloated After Eating (Even When You Eat “Healthy”).
For decades, addressing hormonal health issues has often involved a great deal of speculation. Symptoms without identifiable causes. Laboratory tests indicated normal results while feeling anything but normal. Advances in our understanding of the gut-hormone axis now offer us a scientifically-supported mechanism for identifying specific factors contributing to problems that have challenged both physicians and their patients for generations.
Identifying your unique gut microbiome is not the culmination of your journey toward precision. Rather, it represents the initiation of a far more accurate process.
LONGENY’s truGut360 is a state-of-the-art gut microbiome evaluation, targeted specifically at Indian consumers. truGut360 evaluates multiple aspects of a consumer’s gut microbiome, including microbial diversity; inflammation biomarkers; metabolic pathway integrity; immunological communication between the gastrointestinal tract and systemic immune cells; and early warning signs for long-term hormonal and metabolic disorders – via a non-invasive at-home sampling procedure sent as a personalized digital health report.
If you’ve lived with inexplicable fatigue, PCOS symptoms, thyroid irregularities, hormonal imbalance, or low testosterone – and standard laboratory tests have provided little clarity – this marks the point where things become real.
|
Discover What Your Gut Is Telling Your Hormones Start with truGut360™ – the test that sees what blood tests miss. |
References
[1] Sender R et al. Revised estimates for the number of human and bacteria cells in the body. PLOS Biology, 2016.
[2] Pakpahan C et al. Potential relationship of the gut microbiome with testosterone level in men: a systematic review. PeerJ, April 2025.
[3] Kumari N et al. From Gut to Hormones: Unraveling the Role of Gut Microbiota in Estrogen Modulation. Molecular Nutrition & Food Research, 2024. (Magadh University, India)
[4] Hanna A et al. Systematic review of gut microbiota composition and PCOS. Frontiers in Microbiology, May 2025.
[5] Mei et al. Gut microbiota: an emerging target connecting PCOS and insulin resistance. PMC, 2025. (70% insulin resistance figure)
[6] Nidhi R et al. Prevalence of PCOS in Indian adolescents. Journal of Pediatric and Adolescent Gynecology, 2011.
[7] Thyroid disorders in India: An epidemiological perspective. Indian Journal of Endocrinology & Metabolism / PMC. (42 million figure)
[8] Ruggeri RM et al. The relationship between the gut microbiota and thyroid disorders. Nature Reviews Endocrinology, 2024.
[9] Gut Microbiota for Health. Key advances in gut microbiome research during 2025. January 2026.
[10] Bertollo AG et al. HPA and gut-brain axes in depression. Frontiers in Neuroscience, 2025.
[11] Anil K.C., Founder & CEO, LONGENY. Quoted in Deccan Chronicle, December 2025.
[12] LONGENY / MyBioma launch announcement. Express Nutra, December 2025.

Anil K.C. is the founder of LONGENY, a precision health platform focused on extending healthspan, and longevity, through science-backed diagnostics, nutrition, and personalized care. A serial entrepreneur and host of the Brighter100 podcast, he translates complex longevity science into clear, actionable insights.

Anil K.C. is the founder of LONGENY, a precision health platform focused on extending healthspan, and longevity, through science-backed diagnostics, nutrition, and personalized care. A serial entrepreneur and host of the Brighter100 podcast, he translates complex longevity science into clear, actionable insights.
