
If you have ever said, “I get acidity,” then you are not alone. In India, “acidity” is a common term that includes all types of chest burning, nausea, and bloating. The problem, however, is that in many cases, acid reflux and GERD are not due to having too much acid. The real issue is when acid (and possibly other stomach contents) move up into the esophagus, where they do not belong.
This is why many individuals continue to take quick fixes or continue to take long courses of medications that suppress the production of acid, yet experience their symptoms. If you only reduce your acid levels but pay no attention to the timing of your meals, the size of your meals, how full your stomach feels, your sleeping position,or how bloated your stomach may be, then reflux typically will recur. Understanding your gut microbiome test India can be a pivotal step in identifying why these symptoms persist.
This article is for you, or for you to share with someone else who may be experiencing some of the symptoms listed below:
Acid reflux occurs when stomach contents move up into your esophagus. Your stomach can take the heat (of acid); your esophagus cannot. This is why acid reflux can be so painful. It causes burns, irritation, and a sour or bitter taste.
GERD(Gastroesophageal Reflux Disease) is acid reflux that becomes persistent and/or damaging. In everyday life, GERD is considered to occur when reflux happens frequently (at least 2+ times/week) and affects your daily activities, such as sleep, work, exercise, or mealtime, or causes complications/inflammation (in some cases, seen during evaluation).
Think of it this way:
• Reflux = occasional backflow
• GERD = repetitive backflow that requires a management strategy
An additional distinction: symptom severity does not directly correlate with tissue injury. Some individuals will experience intense symptoms while their tissues appear relatively healthy; others will present with significant inflammation and minimal discomfort. A good treatment approach should address both immediate relief of symptoms and reduction in future reflux events.
Reflux will manifest differently in each individual. For some, it is like the classic “burn.” For many, it feels like it is located in the throat.
Common acid reflux / GERD symptoms:
• Heartburn: burning in the middle portion of the chest after meals
• Regurgitation: sour/bitter fluids moving upward into the throat or mouth
• Pain/discomfort that is exacerbated by reclining/lifting shoulders
• Frequent belching or an uncomfortable “heat” in the top part of the abdomen
• Disrupted sleep due to burning/sour fluids in the throat
Silent reflux/LPR(laryngopharyngeal reflux) symptoms
You may have little/no heartburn, but the refluxate has irritated your throat/voice box:
• Frequent throat clearing
• Hoarse or tired-sounding voice
• Sensation of a “lump” in the throat
• Chronic dry cough, especially after meals or at night
• Feeling of “postnasal drip” without evidence of sinusitis
If you experience difficulty swallowing, food gets stuck, vomit blood, pass black stool, persistent vomiting, unexplained weight loss, anemia/severe fatigue, or chest pain accompanied by shortness of breath/diaphoresis, contact a physician immediately.
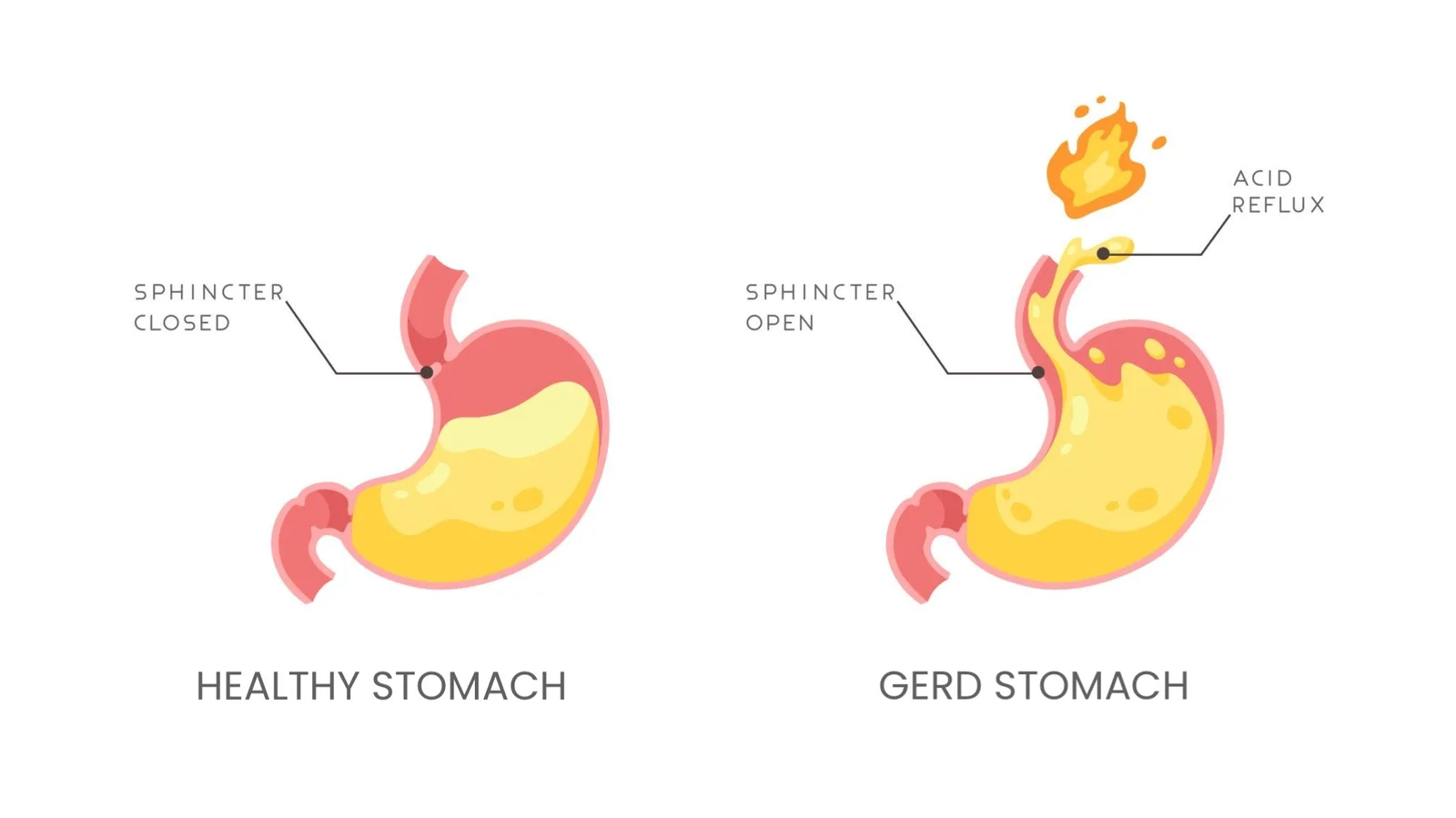
Most people believe that reflux occurs simply because the stomach produces “more acid” than usual. However, in reality, reflux typically occurs due to the presence of acid in an inappropriate location. While the stomach is designed to produce acid, the esophagus is not.
1) Poor function of the valve (LES)
The LES (Lower Esophageal Sphincter) is the muscle ring between the esophagus and the stomach. When the LES relaxes too frequently or weakens, stomach contents can rise.
2) Increased pressure forces the contents upward.
Abdominal pressure increases when large meals are consumed, tight clothing is worn, gas builds in the digestive system, constipation develops, or fat accumulates in the midsection of the body. These conditions force the stomach contents upward through the weakened valve.
3) Timing exacerbates the situation.
Symptoms tend to peak when the patient lies down shortly after eating. Heavy, late dinners are common triggers, as gravity ceases to help at bedtime.
4) Sensitivity and Non-Acid Reflux Exist.
There are people who experience mild reflux that is either mildly acidic or nonacidic, or whose esophagi are overly sensitive. This explains why patients may still have symptoms even though their acid levels have been reduced.
A hiatal hernia (a portion of the stomach slides upward) may weaken the barrier, particularly at night.
Indian food is not “bad” for reflux. More often, the problem lies in the combination we all too often have: late-night eating + large portions + plenty of oils/frying + a lot of stress.
Reducing oil content and portion sizes will be helpful for most people who experience reflux, far more so than completely removing all spices/masalas. Focusing on your overall gut health can help you adapt these habits without feeling like you have to eliminate every food you enjoy.
Late-night eating is perhaps the biggest cause. Eating close to bedtime and then lying down shortly thereafter makes it much easier for reflux to occur. Changing this one thing, to finish dinner 2 to 3 hours before bedtime, can make a huge difference.
For many people, spice is not the villain, but rather the fat load that comes with it. Frequently, the fat load associated with spicy foods (fry tempering, heavy creamy gravies, heavy biryani) is what irritates an already inflamed esophagus.
Reducing oil content and portion sizes will be helpful for most people who experience reflux, far more so than completely removing all spices/masalas.
Chai/coffee may also exacerbate symptoms in certain individuals, particularly if consumed on an empty stomach or later in the day. Drinking chai/coffee post-meal, in smaller servings, and avoiding consuming fried snacks with them is recommended.
Lastly, bloating and constipation are common with irregular meal times, low fiber intake, dehydration, and a sedentary job. These factors increase intra-abdominal pressure and worsen reflux. Steady bowel movements and post-prandial walking contribute to reflux relief far more than most realize.
The gut microbiome does matter, and for many individuals, it is the unaddressed factor in their persistent reflux. However, the useful middle ground is as follows: the microbiome rarely functions in isolation.
The microbiome generally affects reflux through gas/pressure, motility, inflammation, and food tolerance, which is precisely where proper testing and personalized care can be most beneficial.
When the gastrointestinal system produces excess gas (stool backup), the abdominal cavity expands. Increased abdominal pressure creates increased pressure under the Lower Esophageal Sphincter (LES) valve, which increases the likelihood of retrograde flow after meals and at night.
This is why reflux is frequently accompanied by:
a. Postprandial bloating with “healthy” foods (certain legumes, onions/garlic, wheat, large fruit portions)
b. Constipation or irregular bowel habits
c. Feeling excessively full quickly
Your gut bacteria influence both digestion and movement within the gastrointestinal tract. Sluggish motility of food and contents in the stomach and upper part of the gastrointestinal tract results in a prolonged period of time during which reflux episodes are more frequent. Factors such as stress, inadequate sleep, and consumption of highly processed foods can negatively affect this loop.
Can Amplify Symptom Sensitivity
Even minimal reflux episodes can be perceived as extremely uncomfortable if the upper gastrointestinal tract is either inflamed or hypersensitive. The presence of irritation in the upper GI tract due to diet, infection, or imbalance of the microbial population can enhance the severity of the symptoms experienced and potentially prolong the duration of flares.
Microbiome and GI testing is not about achieving a “perfect score”. Rather, it’s about identifying patterns that change your approach. Testing can be helpful when:
Good testing can guide whether the primary focus of the treatment should be on improving motility/constipation, managing fermentation/gas, or repairing an inflammatory gut lining. Additionally, good testing can provide personalized nutrition recommendations (types of fiber, tolerated amounts of fermented foods, ideal meal composition), and whether a clinician-guided assessment is warranted to evaluate for issues such as H. pylori (if appropriate) or other gastrointestinal contributors.
To put this into perspective, there are essentially 2 types of issues with GERD;
During an active episode of symptoms, the primary goal is to provide rapid relief and to minimize the number of episodes of symptoms per day. The interventions listed below are quick, simple, and will have the greatest impact on minimizing reflux and its associated symptoms.
The first step is to utilize gravity to prevent gastric reflux. Finish dinner 2-3 hours prior to bedtime. If you have nocturnal symptoms, sleep on your left side and consider elevating the head of your bed (wedges/risers are more effective than stacked pillows).
Reduce your “rebound” from 2 to 3 days. Eat smaller portions, less oil/fats, and a lighter dinner than your lunch. Eliminate all known triggers temporarily. These include fried foods, large amounts of gravy, alcohol, late-night desserts, carbonated beverages, and mint. Mint has been shown to relax the lower esophageal sphincter (LES) in some individuals.
Move after mealtime. A 10 to 15-minute walk after meals can enhance motility and decrease postprandial bloating and pressure.
Alginates (after meals and at bedtime) may provide additional relief. Alginates create a raft-like barrier that can help prevent the backflow of stomach contents and are beneficial regardless of the presence of acidic or non-acidic reflux.
If symptoms occur daily, disrupt your sleep, or last longer than a few weeks, do not continue to self-treat. Seek a consultation to determine the correct type of reflux you are experiencing (acid, non-acid, hypersensitive) so you can receive treatment based on your specific condition.
During episodes of reflux, many people turn to readily accessible treatments. While these remedies can provide short-term benefits, it’s helpful to understand which treatments are available without a prescription and those that should only be used under a clinician’s direction.
Antacids are the most commonly used OTC treatments. Antacids work immediately by neutralizing the existing acid in the stomach, reducing the burning sensation. Since antacids provide only immediate relief, symptoms tend to recur. Therefore, if you find yourself requiring antacids multiple times a day, take this as a sign. Either your triggers (late evening meals, large meals, bloating/constipation/waist pressure) need to be tightened, or you should seek medical evaluation.
H2 blockers and PPIs are acid-reducing agents that are typically prescribed for more frequent or prolonged symptoms. Both H2 blockers and PPIs are medications that are generally best treated with a physician’s oversight, since the appropriate medication selection is dependent upon your symptom frequency/duration/risk factors, and whether you have any red flag symptoms. Additionally, these medications require ongoing monitoring to avoid long-term use.
In general, think of antacids as providing occasional rescue and stronger acid suppression (H2 blockers/PPIs) as being part of a medically-supervised plan, particularly when symptoms occur frequently, nightly, or consistently when discontinued.
Reflux can be resolved by decreasing the frequency of reflux episodes and the intensity of each episode. The simplest strategy to achieve these goals is to target your largest contributing factor first.
Begin with the big three. Timing, portion size, and fat load. Try finishing dinner early, eating smaller portions, and eating a light dinner compared to lunch. Many people find this strategy provides more benefit than identifying and avoiding a single food item.
Next, make your nights reflux-free. Do not lie flat after eating. Sleep on your left side and elevate the head of your bed using wedges or risers to prevent nocturnal reflux.
Once you’ve made these changes, eliminate the guesswork regarding what you’re sensitive to. For one week, maintain similar meals and evaluate one food-related variable at a time, such as chili spice, amount of oil, coffee/chai timing, carbonation, or late snacks. Look for patterns such as “late + heavy + fried = flare”, allowing you to make educated decisions to avoid your problem foods.
Lastly, address the pressure multipliers: bloating and constipation. Generally, hydration, progressive addition of fiber, cooked meals during episodes of flare-ups, and a brief post-prandial walk can alleviate pressure and associated reflux.
When symptoms continue to occur, a personalized approach – diet + diagnostic assessment of the gut (testing) can transition you from a trial-and-error model to a model that will allow you to sustainably manage your symptoms.
You might have occasional heartburn. However, chronic reflux could be an ongoing issue that doesn’t need to be treated by yourself, especially if you’re experiencing this frequently, worsening, or changing.
There are a number of red flag signs that should prompt you to see a doctor. These would include difficulty swallowing, feeling like food is sticking in your throat, painful swallowing, vomiting blood, black stools, persistent vomiting, unexplained weight loss, severe fatigue/anaemia, or chest pain that occurs along with breathlessness/sweating.
If your symptoms occur daily, disrupt your sleep, or continue to return even after you’ve made some lifestyle changes, your health provider may suggest you undergo diagnostic testing. Some of the most commonly used diagnostic tests include:
It is here that a gut lens can also help: if there is strong evidence that reflux is related to bloating, bowel changes, etc., then the addition of reflux evaluation with targeted testing of the gut/microbiome will likely make your treatment plan more specific.
For many individuals, reflux is perceived as an “acid problem,” however, in reality, it is primarily a barrier-and-pressure problem. How well does the Lower Esophageal Sphincter (LES) valve function? What amount of abdominal pressure develops throughout the day? What time do you eat? How does your body respond when you are having a flare?
A couple of simple adjustments often provide the greatest results in terms of reducing symptoms: eating your largest meal early in the day, consuming smaller portions, decreasing the amount of fried fat you consume at night, taking a short walk after each meal, and improving your sleeping position. Additionally, if you experience bloating or constipation, treating these factors often has a positive effect on the frequency of your reflux. Finally, when you continue to experience symptoms, testing focused on the gut can assist you in identifying what is causing your gas, motility problems, or food intolerance so that you don’t find yourself in a state of trial-and-error.
If you’ve been experiencing frequent reflux, nighttime symptoms, or recurring “acidity” despite making the basic lifestyle adjustments, treat it as a warning sign rather than something that cannot be reversed.For more information on clinical guidelines, you can review the Mayo Clinic’s overview of GERD diagnosis.
By using the right combination of root-cause assessment, personalized nutrition recommendations, and long-term habits, most people can effectively reduce their episodes and get back to feeling normal.
If you’d like to develop a customized plan that includes targeted diagnostic testing of the gut in conjunction with nutrition guidance based upon your individual needs, LONGENY can assist you in identifying your personal drivers and creating a strategy that you can realistically follow.

Anil K.C. is the founder of LONGENY, a precision health platform focused on extending healthspan, and longevity, through science-backed diagnostics, nutrition, and personalized care. A serial entrepreneur and host of the Brighter100 podcast, he translates complex longevity science into clear, actionable insights.
